Almost all new parents go through it: the distress of hearing their child scream at the doctor’s office. They endure the emotional torture of having to hold their child down as the clinician sticks them with one vaccine after another.
“The first shots he got, I probably cried more than he did,” said Remy Anthes, who was pushing her 6-month-old son, Dorian, back and forth in his stroller in Oakland, California.
“The look in her eyes, it’s hard to take,” said Jill Lovitt, recalling how her infant daughter Jenna reacted to some recent vaccines. “Like, ‘What are you letting them do to me? Why?’”
Some children remember the needle pain and quickly start to internalize the fear. That’s the fear Julia Cramer witnessed when her 3-year-old daughter, Maya, had to get blood drawn for an allergy test at age 2.
“After that, she had a fear of blue gloves,” Cramer said. “I went to the grocery store and she saw someone wearing blue gloves, stocking the vegetables, and she started freaking out and crying.”
Pain management research suggests that needle pokes may be children’s biggest source of pain in the health care system. The problem isn’t confined to childhood vaccinations either. Studies looking at sources of pediatric pain have included children who are being treated for serious illness, have undergone heart surgeries or bone marrow transplants, or have landed in the emergency room.
“This is so bad that many children and many parents decide not to continue the treatment,” said Stefan Friedrichsdorf, a specialist at the University of California-San Francisco’s Stad Center for Pediatric Pain, speaking at the End Well conference in Los Angeles in November.
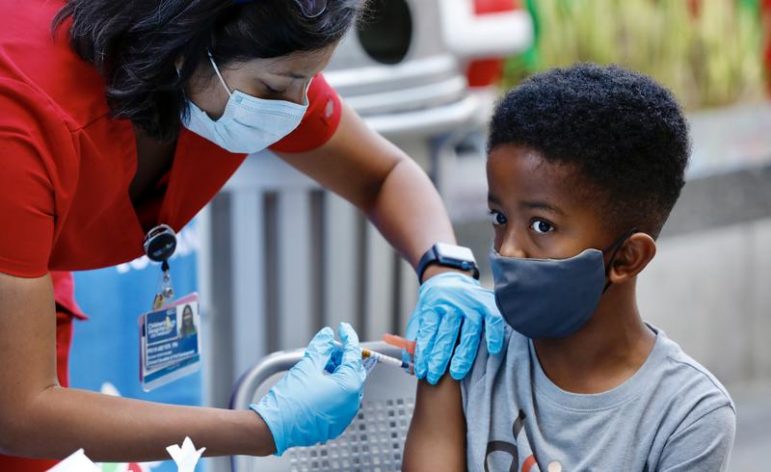
The distress of needle pain can follow children as they grow and interfere with important preventive care. It is estimated that a quarter of all adults have a fear of needles that began in childhood. Sixteen percent of adults refuse flu vaccinations because of a fear of needles.
Friedrichsdorf said it doesn’t have to be this bad. “This is not rocket science,” he said.
He outlined simple steps that clinicians and parents can follow:
- Apply an over-the-counter lidocaine, which is a numbing cream, 30 minutes before a shot.
- Breastfeed babies, or give them a pacifier dipped in sugar water, to comfort them while they’re getting a shot.
- Use distractions like teddy bears, pinwheels, or bubbles to divert attention away from the needle.
- Don’t pin kids down on an exam table. Parents should hold children in their laps instead.
At Children’s Minnesota, Friedrichsdorf practiced the “Children’s Comfort Promise.”
Now he and other health care providers are rolling out these new protocols for children at UCSF Benioff Children’s Hospitals in San Francisco and Oakland. He’s calling it the “Ouchless Jab Challenge.”
If a child at UCSF needs to get poked for a blood draw, a vaccine, or an IV treatment, Friedrichsdorf promises, the clinicians will do everything possible to follow these pain management steps.
“Every child, every time,” he said.
It seems unlikely that the ouchless effort will make a dent in vaccine hesitancy and refusal driven by the anti-vaccine movement, since the beliefs that drive it are often rooted in conspiracies and deeply held. But that isn’t necessarily Friedrichsdorf’s goal. He hopes that making routine health care less painful can help sway parents who may be hesitant to get their children vaccinated because of how hard it is to see them in pain. In turn, children who grow into adults without a fear of needles might be more likely to get preventive care, including their yearly flu shot.
In general, the onus will likely be on parents to take a leading role in demanding these measures at medical centers, Friedrichsdorf said, because the tolerance and acceptance of children’s pain is so entrenched among clinicians.
Diane Meier, a palliative care specialist at Mount Sinai, agrees. She said this tolerance is a major problem, stemming from how doctors are usually trained.
“We are taught to see pain as an unfortunate, but inevitable side effect of good treatment,” Meier said. “We learn to repress that feeling of distress at the pain we are causing because otherwise we can’t do our jobs.”
During her medical training, Meier had to hold children down for procedures, which she described as torture for them and for her. It drove her out of pediatrics. She went into geriatrics instead and later helped lead the modern movement to promote palliative care in medicine, which became an accredited specialty in the United States only in 2006.
Meier said she thinks the campaign to reduce needle pain and anxiety should be applied to everyone, not just to children.
“People with dementia have no idea why human beings are approaching them to stick needles in them,” she said. And the experience can be painful and distressing.
Friedrichsdorf’s techniques would likely work with dementia patients, too, she said. Numbing cream, distraction, something sweet in the mouth, and perhaps music from the patient’s youth that they remember and can sing along to.
“It’s worthy of study and it’s worthy of serious attention,” Meier said.
This article is from a partnership that includes KQED, NPR, and KFF Health News.