Dr. Shura Alexis Moreno has always been one to count his blessings. Nowadays even more so: Every breath he takes with his new lungs feels like one.
His warm smile is back. He’s chatty and at first glance you wouldn’t imagine that just months ago he was on life support. But the flight of stairs in his home leaves him winded. He still doesn’t have the energy to play his drum set. He’s only recently started to gain some weight after losing 40 pounds while hospitalized.
Ten months after he was diagnosed with COVID-19, Moreno is finally getting some of his physical strength back. Yet mentally, it’s still tough.
“A lot of it is psychological,” he said. “I breathe the same, I feel like they’re my lungs. But every so often, I’ll cough and I get a little shaky. I think ‘wow, I have the lungs of someone else. It feels kind of weird.’”
Moreno is one of more than 200 COVID-19 survivors nationwide who have experienced some of the pandemic’s most devastating health effects — their only shot at survival was a new pair of lungs.
Through September, 26 people whose diagnosis was linked to COVID-19 have received new lungs at California transplant centers, according to the United Network for Organ Sharing. That accounts for 10% of all lung transplants performed in the state so far this year.
Surgeons at California transplant centers told CalMatters that they are increasingly evaluating patients whose lungs were destroyed by the virus, including queries from hospitals in other states. This could potentially mean a longer wait time for non-COVID patients on the lung transplant waitlist.
“We’ve done 40 lung transplants (through September this year) and six out of 40 have been on COVID patients, so that’s 15% of our transplants,” Dr. Pedro Catarino, director of aortic surgery at Cedars-Sinai Medical Center who performs lung and heart transplants.
“It’s not that they (COVID patients) are depriving other patients, but there is definitely new pressure on the waitlist.”
Most severely sick COVID patients — hundreds of people — don’t make the cut for a transplant, surgeons said. Hospitals and doctors turn down patients who are too frail to endure the hours-long surgery or who have other serious underlying medical conditions.
California surgeons also now worry how the lungs of their surviving patients will fare in the long-term: Will those left with scarred lungs need transplants later in life? Only time will tell.
105-degree fever and extremely low oxygen
As a general practitioner who runs Gabriel Medical Center, a small clinic on the busy Olympic Blvd. corridor in East Los Angeles, Moreno — who’s Latino himself — saw how the pandemic devastated many families he serves. Latinos account for 53% of infections and 46% of deaths in California while making up 39% of the population.
But he worried less about his own risk. He said he took all the recommended precautions for masks and physical distancing.
Once an avid cyclist, Moreno was still in good shape. He hit the gym a few times a week, and he didn’t have any health concerns. So when he came down with a fever a week before Christmas, he figured he’d isolate and rest.
But Moreno soon became so weak that walking just a few steps would leave him breathless. On Dec. 22 — two days before he was scheduled to get his first dose of the Pfizer vaccine — he was admitted to the same hospital where he often tends to his own patients. His wife and mother-in-law, who also were running fevers, were admitted with COVID-19 the same day.
“For a few days I waited, and that was probably my big mistake,” Moreno said, noting how overwhelmed local hospitals were in those days during the winter surge.
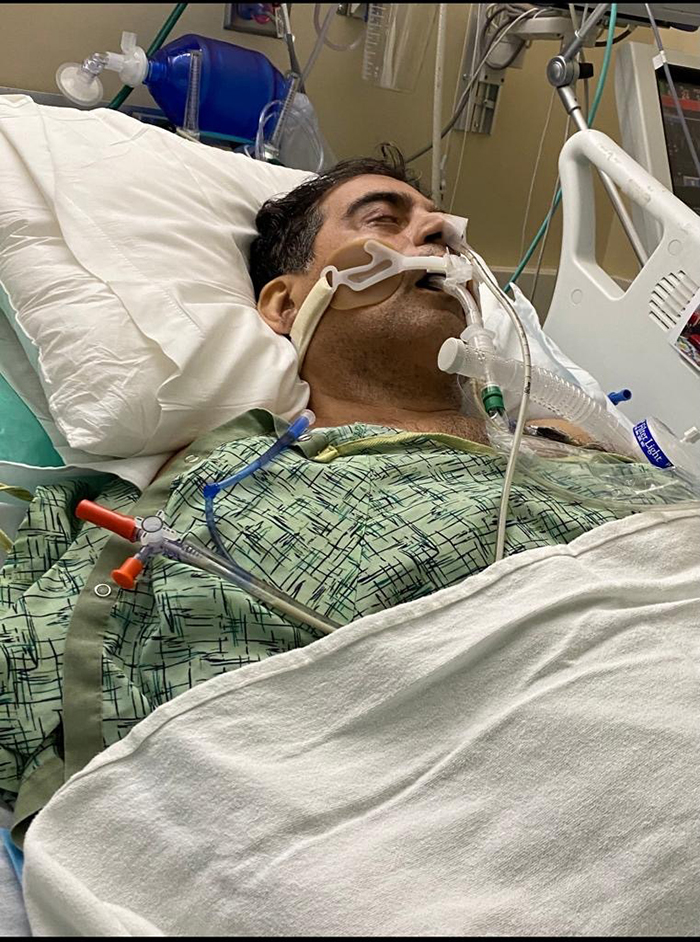
When he arrived at the hospital, he was running a 105-degree fever and his blood oxygen level had sunk to 47% — 95% and above is considered normal for healthy lungs. He remembers at one point pleading to the doctors at Monterey Park Hospital to intubate him — insert a tube into his airways and have a machine breathe for him. “I couldn’t take it anymore,” Moreno said.
His wife and mother-in-law improved, and they were discharged in early January. At one point, Moreno thought he might be in the clear, too. But he’d have one good day in the hospital and then two really bad ones.
On Jan. 16, he was transferred to UCLA Medical Center for more advanced care. He spent his 55th birthday in the intensive care unit, wondering if it’d be his last.
Like many patients whose lungs have been torn up by COVID, Moreno relied for months on oxygen support — first via a ventilator and when that wasn’t enough, a more invasive therapy known as extracorporeal membrane oxygenation (ECMO), in which a machine connected through arteries removes a person’s blood from their body, adds oxygen and then pumps it back in.
The machine is meant to be temporary; the goal is to give the lungs a break to heal. But after almost two months, his lungs showed no improvement. As a last resort, his doctors recommended a double lung transplant.
It was not a decision his doctors made lightly but he was a good fit, according to Dr. Abbas Ardehali, Moreno’s surgeon and director of the UCLA heart and lung transplant program.
“He is a relatively young man, all his other organs were intact and he was ambulatory,” Ardehali said. “Another factor is that he likely acquired this during his professional endeavors, which made us feel we needed to do whatever we could to help him recover.”
To meet the requirements for a transplant, Moreno had to walk at least 20 feet down a hallway. A patient too weak to take steps may be too frail for a transplant, Ardehali explained.
“I felt like I couldn’t even sit on the bed, how was I supposed to walk?” Moreno recalls.
His wife, Tatiana, who for many weeks could only communicate with him via video chat, cheered him on even if she herself struggled to stay optimistic. Colleagues and family sent banners and posters to show their support, while his nurses and therapists played salsa music, Moreno’s favorite, to raise his spirits.
It was the longest 20 feet of his life, and to this day, he’s not sure how he did it.
Once he was cleared, the next step was to wait for a matching donor. Within two days of getting on the waitlist, he had a match. It was a combination of urgency and luck, Moreno said. Patients can wait anywhere from days to years for a matching organ, but usually the sicker the patient is, the higher they end up on the waitlist.
On April 7, three and a half months after he walked into the emergency room, Moreno underwent seven hours of surgery to receive his new set of lungs.
Who qualifies for a transplant
Transplant surgeries are challenging procedures only available in select hospitals. In California, seven medical centers, including three University of California hospitals, transplant lungs, according to the Health Resources and Services Administration. Transplants are usually covered through a patient’s insurance, whether it be private or a public health insurance program like Medicare for seniors or Medi-Cal for low-income residents.
UCLA Medical Center has performed three transplants on COVID patients; Moreno was Ardehali’s first. Three more patients are waiting. And he has received dozens of evaluation referrals from other hospitals across the state, and even the nation, for COVID-19 patients whose lungs have not healed with other therapies.
Surgeons at UC San Diego Health also have seen a significant increase in patient evaluations for transplants during the pandemic. That’s in addition to their non-COVID patients with emphysema, chronic obstructive pulmonary disease or pulmonary fibrosis who also may need transplants.
But the reality is that most virus-afflicted patients end up not qualifying.
“For every candidate we have accepted or considered for lung transplantation, there are another 20 to 30 who have been turned down,” said Dr. Kamyar Afshar, medical director of the Lung Transplant Program at UC San Diego Health.
His team performed its first COVID lung transplant on a 56-year-old man in June.
The ideal candidate’s only medical issue is lung failure — meaning the person would have to be otherwise healthy. Because of the scarcity of organs, surgeons prioritize patients who are very ill but whose bodies show promise of making a full recovery with a transplant.
“When you’re saving the life of one person, you are also taking the lung from someone else, so we want to make sure we’re not doing a futile procedure,” Ardehali said.
COVID-19 can prompt a spectrum of lung conditions, from pneumonia to ruptures and clots in the lungs. If a COVID-19 patient is being considered for a transplant, it’s because that person is very sick, so they will likely end up at the top of the list.
Who gets a new set of lungs first is up to the organ wait list’s algorithm. Patients with lung failure are assigned what’s known as a lung allocation score from zero to 100. The sicker the patient, the higher the score.
“The score is more valuable (to get access to a new lung) than the time you’ve been on the list,” said Dr. Scott Atay, a thoracic surgeon at Keck Medicine of USC. Blood type and distance from the donor hospital also play a role in how quickly someone gets a match.
The best protection against these extreme cases is getting the vaccine, Afshar said. “I think a lot of patients think this is going to be like another common cold, and for a lot of people, they may be asymptomatic or have very mild cases, but in the extremes, it’s a lot worse,” Afshar said. “We’re here to provide a certain service and hope, but if you can prevent it, why not?”
The virus has been the most devastating to seniors — people 65 and older account for 72% of the COVID-19 deaths in California.
But many younger and seemingly healthy people like Moreno have also experienced severe cases. The nation’s first patient with COVID-related lung transplant was a 28-year-old woman in Chicago last summer. A 24-year-old Georgia man made headlines this spring when he, too, underwent a double lung transplant.
Doctors don’t know why some healthy people like Moreno suffer extreme lung damage while most others escape it. They have some theories: greater viral loads and genes, for example, could play a role.
Returning home
After he was discharged in early May, Moreno has been slowly finding his way back to a routine. His days start off with a cocktail of medications, which for the first couple of months post-surgery included about 20 different drugs. He is slowly weaning off most of them, but at least five he’ll take for life.
Anti-rejection medications prevent his body from attacking his new lungs, but they weaken his immune system and leave him more vulnerable to becoming ill from infections. That means Moreno must now be even more cautious: avoiding crowds, always wearing a mask in public and keeping up with booster shots. He received his first dose in July, three months after his surgery. The state as of Sept. 30 requires health care providers to be vaccinated.
Still recovering, his days today are filled with reading, watching the news and Netflix, and taking walks with his wife and 13-year-old son Gabriel — a stark contrast to the demanding schedule he had a year ago. He’ll do 30 minutes on the treadmill and can lift light weights as part of his physical therapy.
Moreno’s ordeal had repercussions on his entire family. Gabriel was often too sad to do Zoom school, so he’d skip it. Tatiana was overwhelmed — balancing his care, overseeing their clinic and caring for their son, who she worried was becoming depressed.

She often went without sleep playing different scenarios in her head. And every time the hospital called, she’d panic, thinking they were calling to inform her that her husband had died.
“When they first told me about the transplant, that day I didn’t sleep, looking up what exactly a transplant meant,” Tatiana said.
She discovered that patients can live up to 10 years after a lung transplant — although some have lived longer. Research shows 59% of transplant patients will live past five years.
Tatiana cried that night thinking 10 years would not be enough. She found some comfort when she thought about time in the form of her son’s birthdays: In 10 years, Gabriel will be 23. At least he’d be an adult, she thought.
Last month, Moreno returned to his clinic a couple of times a week, mostly for administrative work. He’s started to see some of his patients, most of them via telehealth but some in person. His plea to anyone who will listen: Get vaccinated.
“If it happened to me, a doctor taking all the precautions, it can happen to anybody. That’s my preaching point.”
