In the early weeks of the pandemic, Dr. Lorenzo González, then a second-year resident of family medicine at Harbor-UCLA Medical Center, ran on fumes, working as many as 80 hours a week in the ICU. He was constantly petrified that he would catch the COVID-19 virus and guilt-ridden for not having enough time to help his ailing father.
In April 2020, his father, a retired landscaper, died of heart and lung failure. González mourned alone. His job as a doctor-in-training put him at high risk of catching the virus, and he didn’t want to inadvertently spread it to his family. Financial stress also set in as he confronted steep burial costs.
Now, González is calling for better pay and benefits for residents who work grueling schedules at Los Angeles County’s public hospitals for what he said amounts to less than $18 an hour — while caring for the county’s most vulnerable patients.
“They’re preying on our altruism,” González said of the hospitals. He is now chief resident of family medicine at Harbor-UCLA and president of the Committee of Interns and Residents, a national union that represents physician trainees and that is part of the Service Employees International Union.
“We need acknowledgment of the sacrifices we’ve made,” he said.
Residents are newly minted physicians who have finished medical school and must spend three to seven years training at established teaching hospitals before they can practice independently. Under the supervision of a teaching physician, residents examine, diagnose, and treat patients. Some seek additional training in medical specialties as “fellows.”
These trainees are banding together in California and other states to demand higher wages and better benefits and working conditions amid intensifying burnout during the pandemic. They join nurses, nursing assistants, and other health care workers who are unionizing and threatening to strike as staffing shortages, the rising cost of living, and inconsistent supplies of personal protective equipment and COVID vaccines have pushed them to the brink.
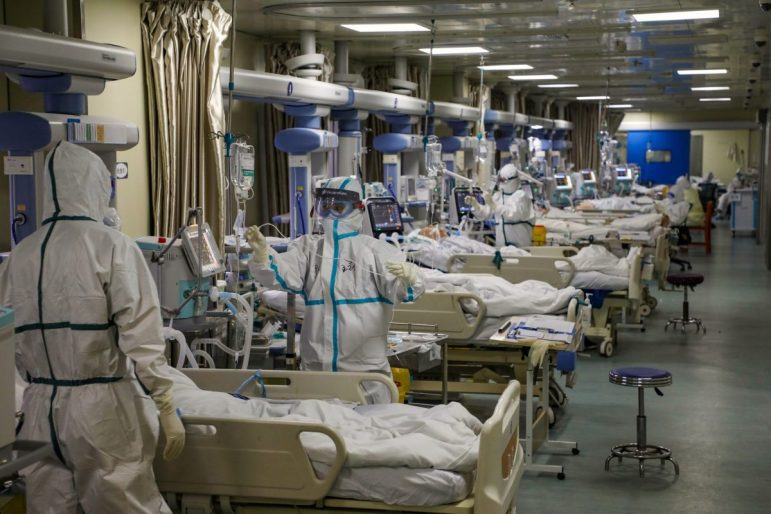
More than 1,300 unionized residents and other trainees at three L.A. County public hospitals, including Harbor-UCLA, will vote May 30 on whether to strike for a bump in their salaries and housing stipends, after a monthslong negotiation deadlock with the county. Since March, residents at Stanford Health Care, Keck School of Medicine at the University of Southern California, and the University of Vermont Medical Center have unionized.
“Residents were always working crazy hours, then the stress of the pandemic hit them really hard,” said John August, a director at Cornell University’s School of Industrial and Labor Relations.
The Association of American Medical Colleges, a group that represents teaching hospitals and medical schools, did not address the unionization trend among residents directly, but the organization’s chief health care officer, Dr. Janis Orlowski, said through a spokesperson that a residency is a working apprenticeship and that a resident’s primary role is to be trained.
Residents are paid as trainees while they are studying, training, and working, Orlowski said, and the association works to ensure that they receive effective training and support.
David Simon, a spokesperson for the California Hospital Association, declined to comment. But he forwarded a study published in JAMA Network Open in September showing that surgery residents in unionized programs did not report lower rates of burnout than those in nonunionized programs.
So far, none of the new chapters have negotiated their first contracts, the national union said. But some of the longer-standing ones have won improvements in pay, benefits, and working conditions. Last year, a resident union at the University of California-Davis secured housing subsidies and paid parental leave through its first contract.
With more than 20,000 members, CIR represents about 1 in 7 physician trainees in the U.S. Executive Director Susan Naranjo said that before the pandemic one new chapter organized each year and that eight have joined in the past year and a half.
Residents’ working conditions had come under scrutiny long before the pandemic.
The average resident salary in the U.S. in 2021 was $64,000, according to Medscape, a physician news site, and residents can work up to 24 hours in a shift but no more than 80 hours per week. Although one survey whose results were released last year found that 43% of residents felt they were adequately compensated, those who are unionizing say wages are too low, especially given residents’ workload, their student loan debt, and the rising cost of living.
The pay rate disproportionately affects residents from low-income communities and communities of color, González said, because they have less financial assistance from family to subsidize their medical education and to pay for other costs.
But with little control over where they train — medical school graduates are matched to their residency by an algorithm — individual residents have limited negotiating power with hospitals.
For unionizing residents seeking a seat at the table, wage increases and benefits like housing stipends are often at the top of their lists, Naranjo said.
Patients deserve doctors who aren’t exhausted and preoccupied by financial stress, said Dr. Shreya Amin, an endocrinology fellow at the University of Vermont Medical Center.
She was surprised when the institution declined to recognize the residents’ union, she said, considering the personal sacrifices they had made to provide care during the pandemic.
If a hospital does not voluntarily recognize a union, CIR can request that the National Labor Relations Board administer an election. The national union did so in April, and with a certified majority vote, the Vermont chapter can now begin collective bargaining, Naranjo said.
Annie Mackin, a spokesperson for the medical center, said in an email that it is proud of its residents for delivering exceptional care throughout the pandemic and respects their decision to join a union. Mackin declined to address residents’ workplace concerns.
Dr. Candice Chen, an associate professor of health policy at George Washington University, believes that the federal Centers for Medicare & Medicaid Services also bears some responsibility for residents’ working conditions. Because the agency pays teaching hospitals to train residents, it should hold the facilities accountable for how they treat them, she said. And the Accreditation Council for Graduate Medical Education, which sets work and educational standards for residency programs, is moving in the right direction with new requirements like paid family leave, she added, but needs to do more.
How far these unions will go to achieve their goals is an open question.
Strikes are rare among doctors. The last CIR strike was in 1975, by residents at 11 hospitals in New York.
Naranjo said a strike would be the last resort for its L.A. County members but blamed the county for continuously delaying and canceling bargaining sessions. Among its demands, the union is calling for the county to match the wage increase granted to members of SEIU 721, a union that represents other county employees, and for a $10,000 housing allowance.
The union’s member surveys have found that most L.A. County residents report working 80 hours a week, Naranjo said.
A spokesperson for L.A. County’s Department of Health Services, Coral Itzcalli, thanked its “heroic” front-line workforce for providing “best-in-class care” and acknowledged the significant toll that the pandemic has taken on their personal and professional lives. She said limits on hours are set by the Accreditation Council for Graduate Medical Education and that most trainees report working “significantly less” than 80 hours a week.
Jesus Ruiz, a spokesperson for the L.A. County Chief Executive Office, which manages labor negotiations for the county, said via email that the county hopes to reach a “fair and fiscally responsible contract” with the union.
Results of the strike vote are expected to be announced May 31, the union said.
