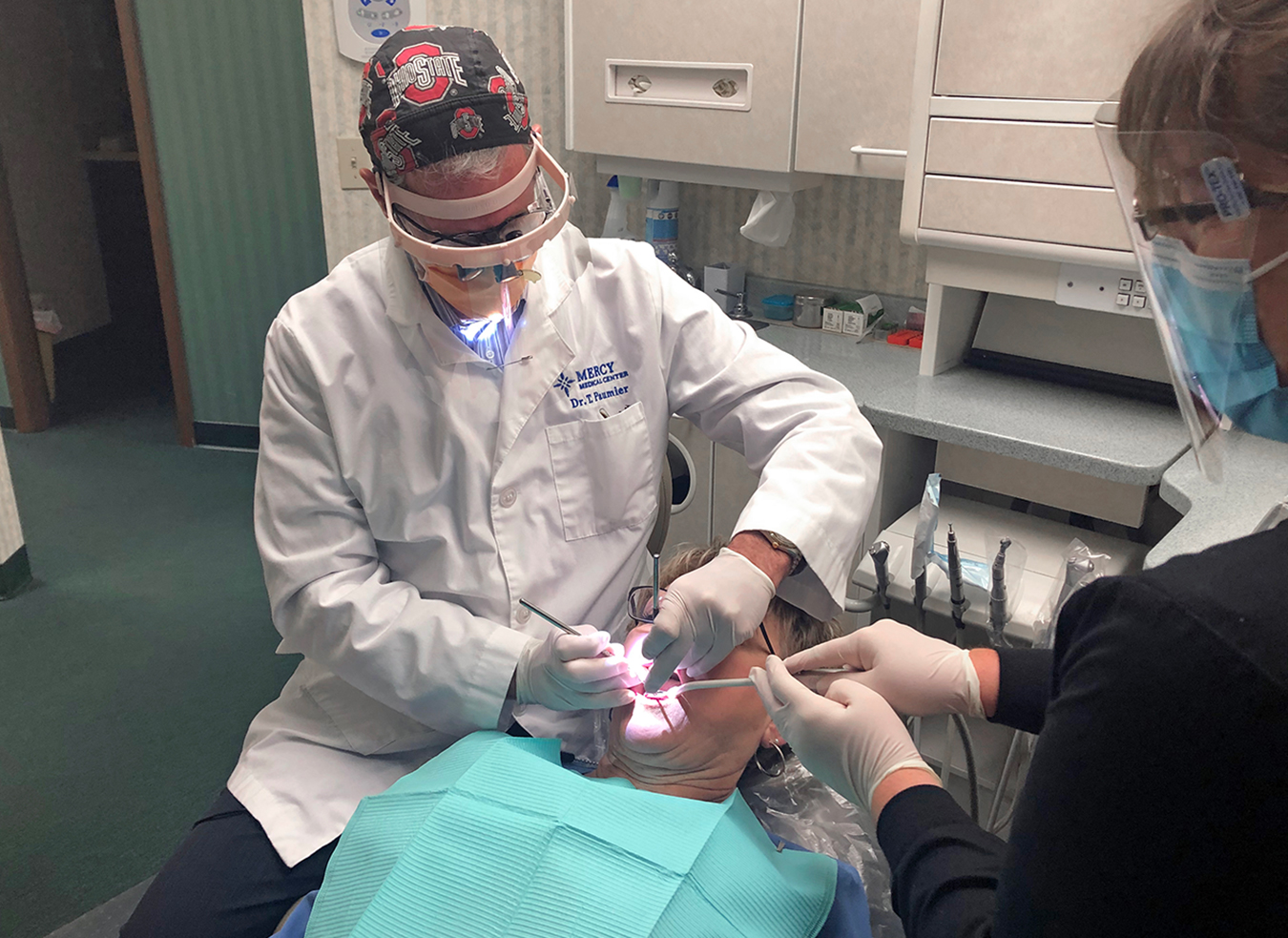
Most states ordered dental offices to close except for emergency patient care when the coronavirus hit the U.S. But the shutdown drilled deep into dentists’ finances, and they have been eager to reopen as states have relaxed their closures.
Tom Peeling wanted his teeth cleaned and wasn’t going to let the coronavirus pandemic get in the way.
Luckily, his six-month regular appointment was scheduled for earlier this month, just days after dental offices were allowed to reopen in Florida for routine services. In late March the state ordered dentists to treat only emergency cases as part of its efforts to keep residents at home and to preserve limited medical supplies, such as N95 masks, that might be needed to treat COVID-19 patients.
Yet for Peeling, 62, of Lantana, Florida, the dental visit was anything but routine. He had his temperature taken upon arrival and was asked to rinse with a hydrogen peroxide solution to reduce germs before the dentist or hygienist looked into his mouth. The dentist and his assistants all wore masks.
Another change: He was the only patient in the office.
Florida is one of 40 states that have allowed dental offices to resume providing routine services following the March shutdown of nonessential businesses in much of the United States when the COVID-19 pandemic began.
The American Dental Association supports dental offices reopening — with added precautions — in states where COVID-19 cases are declining. It notes that patients are better off if they have their regular dental services. The dental group says many dental practices are being hit hard financially because most of their regular patients aren’t coming in for routine care.
But many health experts question whether states are moving too fast.
The federal Centers for Disease Control and Prevention continues to advise patients to limit dental visits to emergencies. The CDC said it has no data yet about the possibility of coronavirus “transmission during dental practice or to determine whether [dental health care providers] are adequately protected when providing dental treatment using standard precautions.”
Matt Crespin, president of the American Dental Hygienists’ Association and a Milwaukee hygienist, also said it’s not time yet. His association believes dentists should postpone all elective and nonemergency care until dental offices have enough equipment such as masks to safeguard all employees and there is more testing to gauge the spread of the disease.
“We have some hygienists who are ready to go back to work and follow the guidance to keep themselves safe and their patients safe,” Crespin said. “But we are hearing from other hygienists worried about going back because appropriate protections are not being put in place” and offices have limited supplies of protective gear.
Infection control experts said patients, dentists and their staffs need to weigh their risks — which vary by where they live, their age and other factors.
“Just because you can be going back to the dentist doesn’t mean you should automatically go,” said Pia MacDonald, an infectious disease expert with RTI International, a nonprofit research institute in North Carolina. She said patients should talk to their dentists about what precautions they are putting in place.
For dental practices, like many other small businesses, the shutdown has been financially devastating. An ADA survey of 17,000 dentists found that by early April more than 9 of 10 dentists said their patient volume was 10% or less of normal, and just under half had stopped paying their employees. Nearly 20% of dentists said they had concerns about sustaining their dental practice if current restrictions are kept in place until the end of June, according to the survey.
“We are going to see more dentists file for bankruptcy if the restrictions go into June,” said Margaret Gingrich, president of the Michigan Dental Association. Like many dentists, Gingrich received a Small Business Administration loan to help her pay rent, utilities and payroll.
Even when dentists get clearance to resume regular visits, it’s uncertain how many patients will postpone out of fear of coronavirus infection. An April survey by the North American Dental Group, which operates 230 dental offices nationwide, found 71% of respondents were uncomfortable going to the dentist for a “non-time sensitive” dental procedure.
“I don’t feel comfortable being in the chair with my mouth open for an extended period of time,” said Marian Hollingsworth, 66, of San Diego.
Adding to their financial woes, many dentists plan to see fewer patients per day to reduce the number of people in their waiting rooms and give staff more time to disinfect areas between cases.
Matthew Roberts, a dentist in Crockett, Texas, who reopened his practice to routine patients last week, said dentists are accustomed to handling germs that can cause infections.
“While we are not used to this novel virus, we deal with infections all the time,” he said. “Patients should have no qualms” about returning.
In addition to wearing N95 masks and gowns, he and his hygienists now use face shields.
When patients arrive at his office, staff members take their temperature to make sure they don’t have a fever, which could signal a COVID infection, and screen them by asking questions about their health.
Roberts said he has been pleasantly surprised that many of his patients have chosen to book appointments once he reopened. He attributed that to his rural county having few COVID cases and patients wanting a return to normal. After being closed for six weeks, Roberts said, he has a backlog of 300 appointments to get through. He’s scheduling patients into September.
Matthew Messina, a spokesperson for the ADA and a dentist in Columbus, Ohio, said that, with added precautions such as having patients wait in their cars instead of small waiting rooms and dentists wearing face shields, people should feel comfortable about going to the dentist even if they are elderly and at high risk for COVID complications.
“The dental office is a safe place for patients,” he said.
MacDonald, the infectious disease expert, recommended, however, that older people consult with their medical doctor about whether a routine dental visit is worth the risk.
“Dentists are uniquely positioned to handle this,” said Thomas Paumier, a Canton, Ohio, dentist who reopened last week. With a shortage of N95 masks, he said, he is using high-quality surgical masks and a face shield.
“Ever since the HIV experience in the 1980s, we treat every patient who walks in the door as potentially infectious,” Paumier said.
Like many other dentists, he donated masks and gloves to area hospitals. But recently, his were returned because they were not needed.
Still, other dentists are concerned about getting adequate supplies. Michael Hoffmann, a dentist and treasurer for the Greater St. Louis Dental Society, said many practices there are “not opening to full capacity — because there’s not enough personal protective equipment.”
He said his own practice has about a month’s worth of supplies. “Once we run out, we’ll have to close our doors until we can get more,” he said.
The society recently used a salesperson Hoffmann had previously worked with to order 100,000 KN95 masks — the European version of N95s — from a supplier in China. But the masks arrived in boxes stamped “nonmedical.”
“When we were trying to fit-check them, they leaked horribly,” Hoffmann said. “Nobody was able to get any kind of seal, and we knew they were fraudulent.”
The group received its money back, and Hoffmann said they will refund the dentists that preordered.
KHN Midwest correspondent Lauren Weber contributed to this story.
Kaiser Health News (KHN) is a national health policy news service. It is an editorially independent program of the Henry J. Kaiser Family Foundation which is not affiliated with Kaiser Permanente.